|
Di seguito tutti gli interventi pubblicati sul sito, in ordine cronologico.
Everything on this site is intended to spoof, parody and satirize.

We make no claims as to the accuracy of our satire.HipsterHitler.com uses the names of public figures for purposes of satire only.
Source: http://hipsterhitler.com
HipsterHitler.com is strictly a parody, satire and humor site, all content herein should be treated as such.

None of the views expressed on this page should be confused with the actual views of the authors, advertisers, the hosting company, any service providers or the owner of this domain name.
Source: http://hipsterhitler.com
Generatia care-ar trebui sa dea socoteala.
Acum 23 de ani aveau 50 de ani. Azi, multi nu mai sunt. Multi au uitat. Multi isi sfarsesc zilele prin spitale cu medici putini. Pensiile lor sunt mici, pentru ca n-are cine sa le mai plateasca. La televizor sunt alte generatii. Viata lor se stinge incet, ca o candela rosie chinezeasca, intr-un cimitir sarac, de tara.
Si totusi, sa ne aducem aminte de ei: sunt cei care au condamnat doua milioane de romani inteligenti si energici si dornici de schimbare la exil.

Sa ne aducem aminte de ei: cei care au votat FSN-ul in 20 mai 1990. Cei care si-au dorit liniste, securitate (in mai multe feluri decat unul), cei care si-au dorit sa apara soarele si imediat dupa el Iliescu, cei care si-au dorit si-au reusit sa puna cu botul pe labe (si imediat pe geamantan si avion) tanara si naiva intelectualitate progresista din Romania. Cei care au detestat golanii. Cei care n-au inteles artistii. Cei care s-au uitat cu scarba la studenti. Cei care au luat cu huo! pe tinerii care voiau libertate. Cei care au aplaudat violenta (da, imi aduc aminte de voi gospodinelor care ii pupati pe mineri!). Cei care s-au inrolat de buna voie intr-o masa de votanti fricosi si prosti (de la varsta, de la salam cu soia, cine mai stie?) si ne-au dat, celor de 20 de ani pe atunci, un certificat simplu si la obiect:
Tara n-are nevoie de tine si de ideile tale. Valea!
Fac parte din acea generatie. Fac parte din ce-a lasat in urma acea generatie, ariergarda ramasilor in tara, naivi si nostalgici si greu de desprins de mirosul Campiei Romane intr-o dupa amiaza de vara. Dar chiar si asa, nostalgic, nu pot sa nu acuz, acum ca sunt batran si inca nu intelept:
I-ati gonit pe cei mai destepti!
Voi, cei care intre 1990 si 1996 ati tinut puterea ca pe o perna pe fata Romaniei evoluate, pana la sufocare, voi care ati saracit spiritual aceasta natiune si i-ati trimis pe fiii ei, pe colegii mei de generatie sa-si caute semeni intre alte neamuri, sa-si caute intelegere intre alte culturi, sa-si caute linistea si cetatenia si uitarea in tari in care jigodiile n-au fost niciodata atat de multe ca aici!
M-am gandit la toate astea zilele astea cand am tot discutat de rezultatele tot mai slabe la BAC, rezultate care ne forteaza sa transformam examenul intr-o farsa, doar, doar n-or pica 80%
Cu riscul de a va jigni, am sa pun intrebarea pe care nimeni n-are onestitatea s-o ridice:
Si daca nu e o problema de educatie? Si daca nu e o grava eroare a sistemului? Si daca nu e decat un lucru simplu, numit in biologie selectie naturala? Si daca Romania de azi, cu notele si cu performanta ei si cu discursul ei public si cu inteligenta ei medie (masurata in statistici medicale de care nu vrem sa stim, nu, nu!) nu e decat rezultatul selectiei fortate de oameni politici ticalosi, in colaborare cu o generatie oarba, acum 20 de ani si mai bine ?
Si daca pur si simplu ce se vede in jur e doar natia care-a mai ramas? Ultimii din tramvai. Cei carora le-a fost frica sa plece, cei care s-au putut obisnui cu mizeria spirituala (mai grava decat cea materiala), cei care si-au zis ca totul trece, cei care prefera sa se descurce decat sa lupte deschis pentru ideile si destinul lor
Ganditi-va la asta cand inca o generatie nu e in stare sa lege trei cuvinte si doua sensuri pe o foaie de hartie la un examen.
Ganditi-va ca povestea acestui esec national a inceput tot pe o foaie de hartie, acum 23 de de ani. Un buletin de vot. Si-o mare, imensa greseala pentru care nu va exista nici o re-evaluare. Nici o contestatie. Nici un examen in toamna istoriei.
Ci doar, poate, un pic mai tarziu, un grup statuar intr-un parc, pe care o sa se aseze porumbeii, ca sa scape de salbaticii nostri urmasi, care-i vor vana cu prastia sa-i manance
Sursa: lucianmindruta.com
De plictiseala, acum cateva zile, am ascultat un post de radio religios, cred ca Vocea Evangheliei sau ceva pe-aproape. N-avea canturi bizantine, deci deduc ca n-avea legatura cu BOR-ul. Desi asta nu e neaparat un defect.

In fine. Las la o parte afirmatiile complet mincinoase in genul de sute de ani stiinta nu face altceva decat sa confirme religia, las si tonul hipnotic, special construit sa inspire emotie si sa rada orice urma de ratiune. Altceva mi s-a parut ingrozitor: la un moment dat, au inceput sa vorbeasca despre Iisus. Cum figura lui e mai mare decat a oricarui lider politic. Cum tot mai multi oameni il urmeaza. Cum in toate tarile lumea stie de el. Cum ideile lui sunt si astazi valabile
Stai! Exact asa spuneau si de Ceausescu! Aceleasi vorbe, aceeasi deferenta, aceeasi lipsa de spirit critic
E ceva in fiinta umana care o sa face sa-si doreasca sa fie dominata? E ceva in noi care tanjeste dupa un model intangibil si perfect, urias si protector, lipsit de defectele si greselile noastre?
Probabil ca da. La fel cum era si-n activistii de partid de acum trei decenii: si ei isi doreau, probabil, pe cineva care sa gandeasca in locul lor. Cateva idei simple, sa nu le transpire creierul. Un drum de urmat unicul sa nu bajbaie incercand sa-l gaseasca pe cel drept
Acum n-as putea spune daca religia e ceausism sau ceausismul era religie.
Cert e ca foarte putini oameni rezista fara sa se inchine la ceva. E mult mai odihnitor sa stii ca acolo sus (sau jos..) e cineva care vegheaza asupra ta decat sa ai sentimentul bazat pe realitate, dar teribil de greu de suportat ca esti complet singur, muritor si absolut neimportant in existenta unui Univers urias si rece.
Tocmai de aceea recomand radioul asta. Pentru ca atunci cand esti suparat, trist, infrant, dat la o parte, el poate sa-ti explice in cuvinte simple ca n-a fost vina ta si ca oricum, ai noroc ca esti crestin. Sau budist sau mahomedan.
Merci, religie. Fara tine nu m-as fi gandit niciodata sa ma resemnez!
Sursa: lucianmindruta.com - Autor: Lucian Mindruta
Mernagh’s court journey started 4 years ago when he was charged for the personal possession and cultivation of cannabis, which Matt used to treat the several illnesses he suffered from including fibromyalgia and scoliosis. Although Matt is one of thousands of Canadians who currently seek medical treatment in the form of cannabis, patients must first request approval by obtaining a medical marijuana license from Health Canada – a policy that Mernagh had not been in compliance with.

With the help of lawyer Paul Lewin, Mernagh’s case was brought before the Ontario Superior Court early last year in an effort to expose the flawed nature of the federal medical marijuana program; a program long scrutinized by eligible patients such as Mernagh for being too inaccessible. After a 3-month long trial, the Ontario Superior Court of Justice ruled in Matt’s favor by striking down the entire regulatory program governing medical marijuana as well as the two sections of the Controlled Drugs and Substances Act that prohibited the production and possession of the plant. The ruling gave the federal government 90 days to improve their medical marijuana program or else cannabis would become legal for anyone to grow or possess.
Since then, the federal government has appealed the ruling and a hearing by the Ontario Court of Appeal has been set for early 2012. With his court date just around the corner, we checked in with Matt for an update on the current situation of medical marijuana in Canada.
TruthOnPot.com: How did you prepare for the trial at the Superior court?
Mernagh: Well, we started working the day after Labor Day and worked all the way through until January. I worked in Paul Lewin’s office almost everyday for a few hours, interviewing potential witnesses who were terminally and chronically ill Canadians that couldn’t get access to the Canadian Medical Marijuana Program. So that’s how I really did the prep-work there, which was 6 months of work while Paul was doing his job.
TruthOnPot.com: Besides the drug dealers profiting from prohibition and this failed policy, who else?
Mernagh: Who else? Obviously, the courts and the police are a big beneficiary of the war on drugs. The police budget is propped up by marijuana money to fight prohibition. We’re easy people to catch! So, the police like to spend the money on that to pump up their numbers. I think the police are one of the biggest beneficiaries of prohibition that there is.
TruthOnPot.com: As a medical marijuana user, what is your opinion on legalizing for recreational use?
Mernagh: I think they should regulate and legalize it for recreational use. Make it a taxed and regulated marketplace. I think that my friends who are recreational users should have quality marijuana where they know what they’re getting – i.e. strains, THC levels, CBD levels, whether it is a sativa, indica, or hybrid. I think they should have the opportunity to buy cannabis like they buy their wine and alcohol.
TruthOnPot.com: Describe how difficult it is in Canada to receive a medical marijuana license and the impact it has on patients?
Mernagh: It’s essentially like winning the lottery. We have less than 1% of doctors in Canada signing paperwork for this Health Canada program. There’s only approximately 10 000 Canadians in it right now. Just to put that number into perspective, there are 60 000 people in Oregon who have their medical marijuana licenses, which is [almost] 1% of their state population. So I think Canada’s doing a terrible job considering the fact that our program is 100% legal, compared to Oregon.
You’re putting a lot of stress on people! You really are affecting people’s health by preventing them from having access to medical marijuana. You’re causing un-due harm in terms of pain and further stress.
TruthOnPot.com: What is your take on legal and medical professionals charging patients obscene amounts of money to receive a legitimate medical marijuana card?
Mernagh: Referrals to a doctor is not what the Law Society teaches, so I think any lawyer that’s involved with referring patients to doctors is probably committing some kind of fraud, if not, a violation of The Law Society Code of Ethics. Because from what I’ve checked, the Law Society does not have a fee for billing people for referrals to doctors. So, these lawyers are middlemen that are charging people to get access to doctors and they are also prohibition propagators. Honestly, they’re as bad as prohibitionists themselves.
In terms of doctor’s charging patients, there is a form to be filled out, so I think there should be a reasonable fee attached to that. I go to my family doctor and the top fee that he charges is $150. So, clearly, medical professionals need to look at what they’re doing in terms of charging a third-party fee.
TruthOnPot.com: How much influence does the United States have on Canada’s legalization efforts right now?
Mernagh: The U.S. has huge influence on Canada’s legalization efforts. In reality, our drug policy for prohibition is completely directed by the U.S. and the UN. You’ll see that in my court factum, which explains that I’m in violation of the ’64 and ‘68 drug-control treaties from the UN, and U.S. drug policies are heavily cited in my factum as the reason Canada has their drug laws the way they are. I think as Canadian citizens, we should be very upset by these things.
TruthOnPot.com: What progress has been made in Canada towards legalization in recent years and how have you contributed?
Mernagh: That’s a great question. Obviously my court ruling, R. v. Mernagh, has struck down the marijuana laws for possession and production and I think that has gone a long way for creating change in our country. It has created discussion, and by the end of this year, Canada may not have a drug policy for personal possession and production of marijuana, because our courts have decided to strike those 2 parts out of the criminal code; that’s the best route we’ve gone so far. Considering we have mandatory minimums, having the courts throw out the marijuana laws, I think, is the best thing we’ve seen in 20 or 30 years.
Source: truthonpot.com
But despite a long and successful career that involved the prosecution of some of Californias worst drug offenders, Judge Gray has an interesting take on the war on drugs he believes that it needs to stop.

Since publicly announcing his position against the U.S. drug war in a 1992 televised press conference, Judge Gray has been instrumental in the movement towards drug policy reform. His book Why Our Drug Laws Have Failed: A Judicial Indictment Of War On Drugs details the many reasons behind his criticism of the drug war, such as the greater availability of drugs to teenagers as well as the softer prosecution of non-drug related offenders that result from drug prohibition. His commentary has also been featured in numerous publications and a wide variety of media including the 2007 documentary American Drug War: The Last White Hope.
Well into his retirement, Judge Gray continues to work tirelessly as an advocate for bringing the drug war to a final end. As such, he was more than willing to answer our questions about his experiences as a former federal prosecutor and how they have shaped him into an outspoken critic of the very same laws that he worked to enforce.

TruthOnPot.com: When was it first clear to you that Americas drug policy was a failed one?
Judge Gray: After I had been on the trial court bench for about 2 and a half years.
TruthOnPot.com: Was there any case or situation you remember in particular?
Judge Gray: Im a former federal prosecutor as well as a former criminal defense attorney in the
Navy and things just started to build up.
There was one case I was involved with in which a really bad man was being prosecuted for being with prostitutes, beating them up, robbing them, and raping them. It turned out that the district attorney had agreed that he would serve such a small amount of time in custody that after everything was over he was taken back into the lock-up and gave out a war whoop.
I thought to myself, Well, he thinks hes won and then I thought, Well, he has won and the reason is that were spending so much time, money and resources on non-violent drug cases were not spending them on robbery, rape and murder. So thats what started me thinking about it and 2 years later I came out publicly about it.
TruthOnPot.com: As a former Superior Court judge, describe how drug prohibition laws are continually putting our children in harms way.
Judge Gray: There are 2 big reasons for this. The first is something I ask high school kids about all the time is it easier for you to get marijuana or alcohol? And the answer is, its easier to get marijuana. Why? Because the illicit marijuana dealers do not ask for ID.
The second reason is if I am an adult drug dealer, how much risk-taking can I buy with 50$ of cash from a teenage boy or girl in the intercity or almost anywhere else? Quite a bit. Because while 50$ is nothing to a drug dealer, to a kid its a fair amount of money. I can recruit all of the young people I want as a cheap source of labor use them as gophers, look-outs, couriers and then, as soon as their reliability is established, I will trust them to go out and sell small amounts of drugs in the communities. Why? Thats easy. I make more money and they make more money.
If you have a 15,16, or 17-year old selling drugs in his or her community, who is that person going to sell to? Theyre not going to sell to adults. Theyre going to sell to their 15 and 16-year old peers, thus recruiting more children to that very lifestyle of drug usage and drug selling that we say were trying to keep away from them and it is caused by the policy of drug prohibition. Today, you do not have students selling alcohol on their high school campuses; but theyre selling methamphetamines or other things pretty much all the time, which is once again caused by drug prohibition.
TruthOnPot.com: Other than drug dealers, what groups of people stand to benefit from the continual enforcement of drug prohibition?
Judge Gray: Well, there are really lots of them. For example, pretty much anybody that builds prisons and anybody that staffs prisons. In the state of California, the prison guards union is probably the strongest political lobby group we have. Theyre winning because were putting all of those non-violent drug offenders in prison.
People that sell burglar alarm equipment and security services, theyre winning. Criminal defense attorneys are winning because theyre getting paid to defend drug dealers. Law enforcement is winning because they keep getting more and more resources to fight the war on drugs; resources that theyre spending on that war and not on robbery, rape and murder.
TruthOnPot.com: In the state of California, public ballot initiatives for a regulated marijuana market (such as the Regulate Marijuana Like Wine campaign) have received growing support. What sorts of things should an average citizen expect to see if marijuana were to be legalized and regulated in states such as California?
Judge Gray: You would see a small increase in the use of marijuana by adults over time. Some of those would come from not using so much alcohol and going to marijuana instead, which, to be honest, would still be a better thing. You would also see people who used to take drugs like methamphetamines come down the ladder and probably use marijuana.
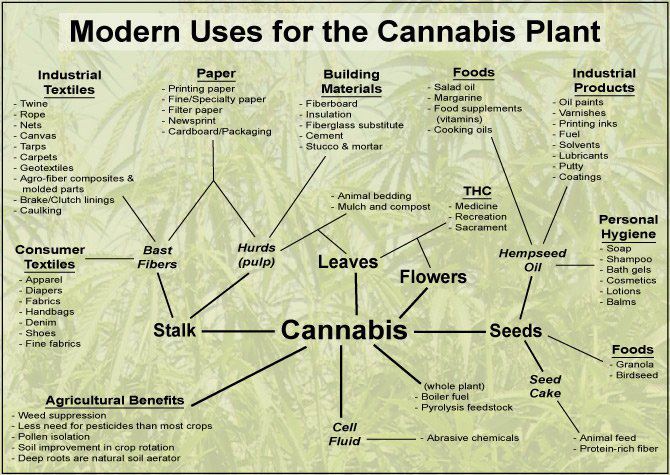
You would also see an enormous increase in the hemp industry. Some people may not know this, but hemp is an industrial product derived from the marijuana bush; the stalk itself has enormous properties and uses that go back thousands of years.
You would also see a lot of tax money coming into the local state and federal governments that is not coming in now. As they say, marijuana is the largest cash crop in California but none of that goes towards taxes, except for medical marijuana dispensaries. So, you would see a great deal more in tax revenue coming into the governments and they would save according to the Attorney General of California tens of millions of dollars that theyre currently spending in trying to enforce this unenforceable system.
TruthOnPot.com: What types of changes to do you see in other countries with regard to drug policy and how is the United States affecting international opinion?
Judge Gray:The United States is running the bus with regard to drug prohibition and if the United States were to change its position, the rest of the world would heave a sigh of relief.
Even still, there are major propositions going on in Latin America right now to regulate and control marijuana, or even heroin and cocaine, because they are the ones that are suffering from the corruption and the violence that is caused by our countrys drug problem. Theyre beginning to see that the only way to reduce the corruption and violence and the only way to get rid of the drug cartels is to regulate and control these substances and theyre well on their way to doing that.
TruthOnPot.com: Youve been a public proponent of drug policy reform for 20 years now. What has changed since you first began to voice your support for this cause?
Judge Gray: There have been 2 sizeable changes. One is for the worse. That is, we are in worse shape today with regard to filling our prisons and the cost of drugs. There are far more drugs in our community today than there were 20 years ago, there are far more people in prison than there was 20 years ago, and the cost of drugs is less today than 20 years ago all of that change is negative.
The positive is that more people are beginning to understand what is going on. More people in the media, more people in the chambers of commerce, even more elected officials are beginning to understand that just because we discuss the regulation and control of these various drugs does not mean that we condone people using them.
They are also beginning to see that drug addiction is a medical problem, not a criminal justice problem. They are beginning to understand that we should bring drug-addicted people closer to medical professionals that can help them and reserve the criminal justice system to control peoples actions instead. If you drive under the influence of any of these drugs (including alcohol), if you beat up your spouse, if you hit somebody over the head with a pool cue; that is a criminal justice issue. People are beginning to understand that as well as the taxes that they are losing by not regulating and controlling marijuana.
Its only a question of time. I tell people that I absolutely guarantee them that we will change away from this failed system and, within 2 years of doing so, almost everybody will join hands and look back and be aghast and astonished that we could have perpetuated this failed system for so long.
Source: truthonpot.com
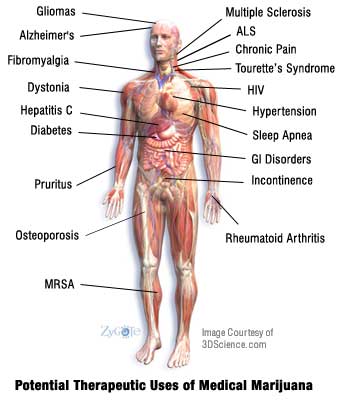
He has seen and experienced its benefits firsthand through his involvement with some of the first clinical marijuana trials to ever be conducted on patients with the painful, life-threatening disorder.

Dr. Abrams currently serves as the chief of Hematology and Oncology at San Francisco General Hospital. In 2006, Abrams took on an additional role as a cancer and integrative medicine specialist at the UCSF Osher Centre for Integrative Medicine at the University of California, San Francisco.
On top of his demanding and accomplished career, Dr. Abrams remains on the forefront of medical cannabis research. Widely respected by patients and doctors alike, TruthOnPot.com was eager to speak with Dr. Abrams about his work in this exciting field of medicine.
TruthOnPot.com: What sparked your interest and involvement with medical cannabis research?
Abrams: It goes back quite a while. I did my training to be a cancer specialist in the 70s, when we didnt have a lot of anti-nausea drugs and many of our patients seemed to benefit from smoking cannabis at that time.
In 1989, I had a partner who died of AIDS after choosing not to take AZT the only anti-retroviral drug available then under my recommendation. I didnt think that it was very good. But he found benefit from smoking cannabis, which he did daily.
In 1992, while I was in Amsterdam for the International AIDS Conference, I saw Mary Ratburn on the CNN headlines news being arrested for bringing cannabis brownies to our AIDS patients at San Francisco General Hospital. She was in her late 60s and brought brownies to our patients so they could eat their food and take their medicine.
When I got back to San Francisco, there was a letter from Rick Doblin founder of the Multidisciplinary Association of Psychedelic Studies (MAPS) suggesting that a clinical trial demonstrating the benefits of cannabis should come from Marys institution. I responded to the challenge and began discussions with the government in hopes of conducting clinical research on marijuana.
TruthOnPot.com: Can you describe the results of the various medical marijuana studies that youve been involved with?
Abrams: The first study that I wanted to do was a study to show that marijuana improved appetite in patients with the AIDS wasting syndrome.
But what I learned was that the National Institute on Drug Abuse (NIDA) which is the only legal source of cannabis in the country has a mandate from Congress to only study substances of abuse as substances of abuse. Meaning that if they figure cannabis is a substance of abuse, they cant provide cannabis or fund studies that are going to try to demonstrate that it has medicinal benefits.
By the time I came to understand this, we already had drugs that were effective in combating the AIDS wasting syndrome. But, there was a possibility that recreational drugs could interfere with the metabolism of the anti-viral therapies.
In 1997, I received funding for my first study which looked at a potential interaction between cannabis (we used dronabinol in this case) and protease inhibitors the potent drugs that were saving AIDS patients lives. We looked at the level of the AIDS virus, the impact on the immune system, the levels of the anti-viral drugs and any changes in weight and appetite. We found that cannabis caused no real problem in any of these instances and, if anything, we saw weight gain in patients with HIV who did not have the wasting syndrome.
In California, we had the University of California Center for Medicinal Cannabis Research (CMCR), which had $3 million a year for 3 years to fund clinical trials investigating the safety and effectiveness of cannabis in various conditions. The first study I did with CMCR funding was again in patients with HIV who had painful nerve damage known as peripheral neuropathy. We did a placebo controlled trial that showed that inhalation of smoked cannabis lead to a decrease in the pain, both from the peripheral neuropathy as well as in an experimental pain model that we did on the patients.
The next study we did was to examine the Volcano Vaporizer as a smokeless delivery system because we knew that people were not enthusiastic about smoking a medicine. We took healthy cannabis smokers and subjected them to 3 different strengths of NIDA cannabis. We found that vaporization produced the same amount of active cannabinoids in the blood stream, that it was actually preferred by the patients, and that it was associated with less expired carbon monoxide, which is a marker of exposure to harmful gases.
The last study that we did was a pharmacokinetic interaction study which involved patients with chronic pain taking a stable dose of sustain-released morphine or sustain-released oxycodone. We subjected them to vaporized cannabis for 4 days and we measured the level of the opioids in their bloodstream before and after exposure to cannabis to see if there was any interaction. We found no significant change in the levels of opioids. If anything, the levels of morphine seemed to decline slightly. But we did see a boost in pain relief despite the slightly lowered levels of opioids. That suggested there was a synergistic interaction between cannabis and the opioid medications that is, 1 + 1 = 5 as opposed to 1 + 1 = 2. Hopefully, the next study we do will be a larger study to confirm the synergistic interaction between the two.
TruthOnPot.com: How do the synthetic cannabinoid medicines compare to vaporized cannabis?
Abrams: Delta-9-tetrahydrocannabinol (THC), which can be obtained in oral capsule form, is just one of over 400 components of the plant. I believe having all the other components of the plant provide the ying and the yang that is, they balance out the negative effects of THC and enhance the positive effects.
Sativex is now also available in Canada and Europe and is in clinical trials in the US. This under-the-tongue spray is a whole plant extract that has some manipulation of the CBD and THC ratios, which some people find quite useful.
TruthOnPot.com: Could the pain-mitigating effects of medical cannabis be applied to any other conditions or disorders?
Abrams: Id recommend it to anybody with pain, the research has already been done there.
I think theres good evidence for its use in helping with nausea and sleep. I often recommend cannabis to my cancer patients for nausea, pain, depression and insomnia, just because I know that it works you dont have to do a clinical trial to prove that.
TruthOnPot.com: In your opinion, is marijuana a viable alternative to current legal substances such as alcohol and tobacco?
Abrams: It was certainly my alternative in college and medical school. Id be a very different person today if I chose alcohol instead of cannabis at Brown University and Stanford University School of Medicine.
Source: truthonpot.com
The main change is to eliminate personal production in favour of licensed commercial producers who would be inspected and audited by Health Canada.
Spokesperson Stéphane Shank said the government just finished a consultation period on the changes last month. The government is now analyzing the results, with a plan to implement the changes by March 31, 2014.

Currently there are three types of medical marijuana licences authorization to possess, personal-use production (can only produce for yourself), and designated-person production (can produce for someone authorized to possess).
The licences to possess marijuana or grow marijuana for yourself require a medical declaration by a doctor. Doctors are supposed to ensure patients have severe pain or other health problems that cannot or should not be treated by a conventional treatment.
Someone with a recent criminal record for drug activity cannot get a licence to grow for someone else. Health Canada requires a criminal conviction to revoke someones licence.
However, Shank said the government cannot readily provide statistics about how many licences have been revoked.
Health Canada has 15 inspectors.
The amount of marijuana someone can produce is based on a specific calculation on the patients medical needs and can vary widely. There are extra steps if the maximum amount is more than 5 grams dried daily.
Those with a licence to produce marijuana for another person can hold two licences, and only four licences are allowed to be used at one address, Shank said.
For more information about the Marihuana Medical Access Program and planned changes visit Health Canadas website.
Source: thespec.com via truthonpot.com
Under this legislation, substances are separated into one of five Schedules (classifications) according to their potential for abuse, accepted medicinal use and international trade laws.
Cannabis is currently classified as a Schedule I substance a position it has retained since the Controlled Substances Act was drafted over 42 years ago.
Schedule I Laws
The classification of a Schedule I controlled substance is assigned to only the most dangerous and least medically useful of drugs, which subjects both researchers and offenders to the highest level of restrictions and penalties that can be administered. For a drug to be placed in the Schedule I category, it must fulfill all three points of the following criteria:
1. The drug or other substance has a high potential for abuse.
2. The drug or other substance has no currently accepted medical use in treatment in the United States.
3. There is a lack of accepted safety for use of the drug or other substance under medical supervision.
Title 21 of the U.S.C. § 812b
Classification of Cannabis
Even at first glance, the definition of a Schedule I substance seems a bit too harsh to be applied to marijuana. In fact, among other drugs that share the same category such as heroine and opiates none can make claim to being a treatment for so many disorders while having no risk for overdose like cannabis can. Although its potential for abuse might still be debatable, an overwhelming amount of scientific evidence gathered over the past few decades has proved the last two points as being grossly inaccurate.
So how has cannabis managed to maintain such a mistaken classification under federal drug policy for all these years? To answer that question, lets look at how marijuana came to be classified as a Schedule I substance in the first place.
National Commission on Marihuana and Drug Abuse
While the Controlled Substances Act was being drafted in 1970, marijuana was placed in its Schedule I category on advice from Assistant Secretary of Health Roger E. Egeberg. In his letter to Harley O. Staggers, Chairman of the House Committee on Interstate and Foreign Commerce, Egeberg made it clear that the classification was meant to be temporary:
Dear Mr. Chairman: In a prior communication, comments requested by your committee on the scientific aspects of the drug classification scheme incorporated in H.R. 18583 were provided. This communication is concerned with the proposed classification of marihuana.
It is presently classed in schedule I(C) along with its active constituents, the tetrahydrocannibinols and other psychotropic drugs.
Some question has been raised whether the use of the plant itself produces severe psychological or physical dependence as required by a schedule I or even schedule II criterion. Since there is still a considerable void in our knowledge of the plant and effects of the active drug contained in it, our recommendation is that marijuana be retained within schedule I at least until the completion of certain studies now underway to resolve the issue. If those studies make it appropriate for the Attorney General to change the placement of marijuana to a different schedule, he may do so in accordance with the authority provided under section 201 of the bill
Sincerely yours, (signed) Roger O. Egeberg, M.D.
The reference to the completion of certain studies now underway was to the National Commission of Marijuana and Drug Abuse, which was created by public law 91-513 for the specific purpose of studying marijuana abuse in the United States.
The Commission was chaired by former Pennsylvania Governor Raymond P. Shafer and consisted of 13 members, 9 of which were handpicked by President Nixon himself. To date, the National Commission on Marijuana and Drug Abuse is the only congressional commission to ever assess marijuana policy.
In 1972, the Commission completed and presented their report entitled Marihuana: A Signal of Misunderstanding to Congress, which detailed their investigation and overall recommendation for marijuana to be reclassified and prohibition to be ended.
Marihuana: A Signal of Misunderstanding
In their report, the commission determined that minor possession offenses should be decriminalized under federal law. Likewise, the Commission recommended that states should also eliminate criminal penalties for minor pot offenses.
[T]he criminal law is too harsh a tool to apply to personal possession even in the effort to discourage use. It implies an overwhelming indictment of the behavior which we believe is not appropriate. The actual and potential harm of use of the drug is not great enough to justify intrusion by the criminal law into private behavior, a step which our society takes only with the greatest reluctance.
The report acknowledged that, decades earlier, the absence of adequate understanding of the effects of the drug combined with lurid accounts of [largely unsubstantiated] marijuana atrocities greatly affected public opinion and labeled the stereotypical user as physically aggressive, lacking in self-control, irresponsible, mentally ill and, perhaps most alarming, criminally inclined and dangerous. However, the Commission found that the drug typically inhibited aggression by pacifying the user
and generally produc[ed] states of drowsiness, lethargy, timidity and passivity.
The findings of the report were met with expected resistance from Congress and were largely ignored by the Nixon Administration. As the infamous white-house tapes would reveal, President Nixon fostered a strong opposition to the Commissions recommendation even before it was released. In 1971 a year before the report was completed Nixon warned Shafer, Youre enough of a pro to know that for you to come out with something that would run counter to what the Congress feels and what the country feels, and what were planning to do, would make your commission just look bad as hell.
And despite the firm recommendation of the federally commissioned report that took years to complete, cannabis retained its classification as a Schedule I narcotic under the Controlled Substances Act, which prevents any person or organization from free access to the cannabis plant whether for recreational, industrial or medical purposes.
To this day, the decision of the Nixon Administration to ignore the Commissions recommendation to end prohibition continues to be upheld by federal policymakers.
Source: truthonpot.com
|